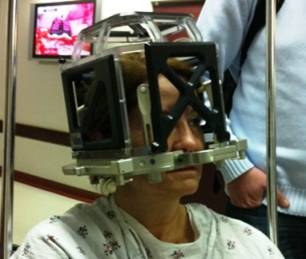
Yael Bossem-Levy, spokesperson for the Hadassah University Medical Center, underwent successful Deep Brain Stimulation surgery to relieve the tremors she suffered from her slowly progressive neurological disorder. Ironically, she had arranged for an Israeli television crew to film Israel’s first Deep Brain Stimulation procedure on a Parkinson’s patient—at Hadassah—many years ago. Here is her touching story, in her own words:
“I don’t remember the exact day my hands began to tremble and neither does anyone close to me, but more than 10 years ago, I was diagnosed as having Essential Tremor, a slowly progressive neurological disorder that is intensified by pressure or anxiety.
The trembling caused no small number of embarrassing situations and difficulties in everyday functioning. Basic activities such as putting on makeup, using a computer mouse and tooth-brushing became genuine tasks. When I was being interviewed by the media, I found that I couldn’t hold the microphone.
Just as I cannot pinpoint the exact onset of the trembling, I don’t know which event or events affected the rate of deterioration. From the day I arranged for the crew to film Dr. Zvi Israel, now head of Hadassah’s Center for Functional and Restorative Neurosurgery, I knew that Deep Brain Stimulation was a possible solution—but the very thought of brain surgery terrified me.
Last year my condition deteriorated even further. After consulting the leading neurosurgeons and movement disorder specialists in the country–Prof. Tamir Ben–Hur, head of Hadassah’s Department of Neurology, who has taken care of me for many years; Prof. Avinoam Reches, head of the Neurology Department’s Center for Parkinson’s Disease and other Movement Disorders; and Prof. Nir Giladi, head of Ichilov Medical Center’s Department of Movement Disorders–my heart told me it was time to go ahead with the surgery.
 There was unanimous agreement that Dr. Israel is the country’s leading expert, the surgeon with the most experience, the man who initiated the procedure in Israel. He introduced me to patients who had undergone the operation and–with his characteristic calm and confidence–he did not withhold any details, including the chances for success and the risks. I decided to think positively, but brain surgery is not “just another operation.”
There was unanimous agreement that Dr. Israel is the country’s leading expert, the surgeon with the most experience, the man who initiated the procedure in Israel. He introduced me to patients who had undergone the operation and–with his characteristic calm and confidence–he did not withhold any details, including the chances for success and the risks. I decided to think positively, but brain surgery is not “just another operation.”
Then the day arrived. Apprehensively, I got into a wheelchair. Dr. Israel and the assistant surgeon started to attach the metal framework to my head. Dr. Israel tied my hair back with a ponytail holder–even in that field, he has a lot of experience because he has four daughters. It was noon when Dr. Israel said: “On target. You’ll feel a shot; it will hurt a lot.” An injection and then another one, and another and another. Some blood dripped down and the tears flowed unbidden. Then, using a CT, Dr. Israel checked to confirm the heavy metal superstructure framework was exactly in place.
In the operating room, Dr. Israel placed my head with the framework inside a fixed device and guided it into place. “Choose the position that’s most comfortable for you,” he instructed, “because you’ll have to stay that way without moving the entire time.”
Prof. Hagai Bergman of the Hebrew University-Hadassah School of Medicine’s Department of Physiology joined us and introduced himself. Of course, I had heard of him. He was responsible for measuring and recording the electrical data from the basal ganglia, the complex structure in the center of the brain linked to initiating and regulating motor commands.
The surgery consists of the bilateral implantation of electrodes that the patient will control with a pacemaker-like device. The electrodes transmit electrical impulses to the affected area of the brain, thus regulating the tremor.
When Dr. Israel cautioned that I would hear the sound of a drill, the fear of God shot through me. They were drilling in my head. I screamed silently for them to stop and clutched desperately at the blanket, seeking consolation. The drilling seemed to go on for an eternity. Even though Dr. Bergman told me in a soothing voice to “think of things you like, beautiful songs,” no matter how hard I tried, I could only hear the sound of the drill.
The atmosphere in the operating room was quiet and totally concentrated as Dr. Israel and the team focused only on their goal–inserting the electrodes in exactly the right spot in my brain.
I heard a screeching noise above my head. There was a slight easing and the clock across from me that had crept forward like a tortoise showed it was now four o’clock. Time to give me the general anesthetic so they could conduct the second part of the surgery, inserting the lead wires under the skin and implanting the pacemaker. You can understand how happy I was that they were going to put me to sleep.
After recovering from the surgery in the Neurosurgery Intensive Care Unit, I spent a weekend in the Neurosurgery Department where the most amazing team of nurses care for complicated patients with unending patience—feeding them, bathing them, and attending to all their needs.
On Friday, Dr. Israel came to the department with the remote control to adjust my electrodes…yes, some adjustment is required before you reach the optimal settings. Everything still hurt but he promised that within two weeks, the pain would pass. He was right.
Two and a half weeks after the surgery, I felt just like new. I’ve gone back to my daily routine but now I am a bionic woman. At night, I put the remote control up against the invisible pacemaker and shut it off to prolong battery life. In the morning, I turn it on again. And I no longer tremble.
I’m proud of our Medical Center. I trust it completely. I underwent the surgery knowing I was putting my head in the hands of Israel’s greatest expert, in the leading institution in Israel– a world leader–in the place that’s my second home.”
