By Devorah Blachor
Jerusalem – An LCD screen faces the nurses’ station at the Pediatric Intensive Care Unit of Hadassah Hospital in Ein Karem, Jerusalem. The screen is divided into seven sections, each one showing the vital signs of a different child on the ward. Each patient is constantly monitored – EKG, oxygen, bloodstream and heartrate. When a blue light flashes on the screen, it means there’s an alarm.
“It’s a matter life and death here,” said Dr. Philip Toltzis, Director of Pediatric Intensive Care. “It’s not like a regular pediatric ward.”
In early November, all seven children in the ward were Palestinian – either from East Jerusalem or the West Bank – and all but one were babies, ranging in ages from two weeks to eight months. The seventh patient was five-years-old.
“A lot of our job is hotel management,” Dr. Toltzis said, joking about a very real challenge facing the ward. “The biggest problem is that there’s not enough room. Too many babies and children and too few beds. Every day, we try to see who can go where – can we move anyone into a different ward? There’s always someone knocking at the door.”
All the babies in the ward were suffering from some variation of heart disease – one from mitral valve regurgitation, another from Shone’s complex, and a third had recently suffered a small cardiac arrest. Dr. Toltzis said that he’s observed a larger proportion of congenital heart disease in the Hadassah ward than what he’s seen in the US, where he also practices. This may be attributed to first-cousin marriages among Palestinians and ultra-orthodox Jews.
Many cases of congenital heart disease can be treated, but one of the challenges facing the Hadassah staff is that there’s often no prenatal screening among ultra-orthodox Jews and in the Palestinian sector. If doctors know the baby has heart disease before it’s born, the child can be monitored and treated accordingly. But because of the lack of prenatal screening, many babies with heart defects are sent home after they’re born, with no awareness that there’s a problem.
The complications often arise days after the birth when the ductus arteriosus closes – which is part of the normal development of a baby. But for some babies suffering from congenital heart disease, when the ductus closes, the serious complications begin. The baby starts to look very ill, because blood isn’t getting to the organs. If the baby does not receive care, she’ll die.
A baby like this will be sent to PICU, and the pressure on the staff is enormous.
“Most people who go into pediatric medicine don’t want to have anything to do with an ICU because of the extreme stress,” said Dr. Toltzis, “But there’s a small number of us who choose this work. “
The result of their work is impressive. Hadassah’s PICU has a 96% success rate. That means that 96 children out of a hundred who come to the ward – and if they’ve come to this ward, they’re in very serious condition – go home.
“What gets done here is the same as what would get done in any top level ICU in the world,” Dr. Toltzis said. “For those of us that came from outside the country, there’s a lot of satisfaction to do this here in Jerusalem.”
Giulia Gallichi Punterello, an Italian immigrant to Israel, was in PICU last year with her two-year-old son Jona who had life-threatening pneumonia.
“They saved my son,” she said. “All the doctors and nurses were so kind. I love all of them.”
Dr. Toltzis pointed to a couch on the ward where PICU’s doctors often spend the night. He said that when he started working at Hadassah two years ago – he also practices at the Rainbow Babies and Children’s Hospital in Cleveland and commutes between the two cities – he was struck by the passion and dedication of the PICU staff.
“Everything possible is done,” he said. “You don’t go into pediatric care to say it’s time to let go. With a kid, it’s never time to let go.”
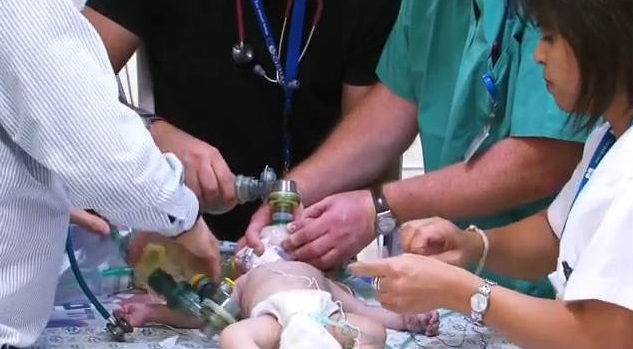
As the babies on the ward struggle for every breath, one of the focuses of the PICU staff is to wean them from mechanical ventilators. If the babies can breathe on their own, they can get transferred to another ward and then go home. Once home, the babies can grow and strengthen, and those that still suffer from heart defects can undergo corrective surgery.
But for some children, the plan isn’t so clear. The five-year-old on the ward suffers from serious seizures caused by ‘short circuits’ in the brain. Since the short circuits aren’t localized in one part of the brain – they’re spread all over – there’s no possibility to remove the section that causes the seizures. The child had to be put in a barbiturate coma to stop the seizures. The prognosis isn’t good.
“We don’t know what will happen with this child,” Dr. Toltziz said. “But we have to keep trying.”
The staff of PICU is fueled by the adrenaline of working in such a high-pressure environment, according to Dr. Toltzis. Every decision is critical. “When it doesn’t work, there’s nothing more horrible. But when it works, there’s nothing better.”
